Why collaboration between Sterile Services and Operating Theatres matters
Across hospitals in Australia, the relationship between the Central Sterile Services Department (CSSD) and Operating Theatres is one of the most critical partnerships in surgical care. Yet many healthcare professionals recognise a persistent cultural divide between the two.
Theatre teams may experience frustration when instruments are delayed or incomplete. CSSD teams often face pressure from late surgical list changes, incomplete instrument returns, or unrealistic turnaround expectations.
But the reality is simple: CSSD and theatres are not separate systems — they are two parts of the same surgical ecosystem.
Improving collaboration between these departments is essential for patient safety, operational efficiency, and staff wellbeing.
Two Departments, One Surgical System
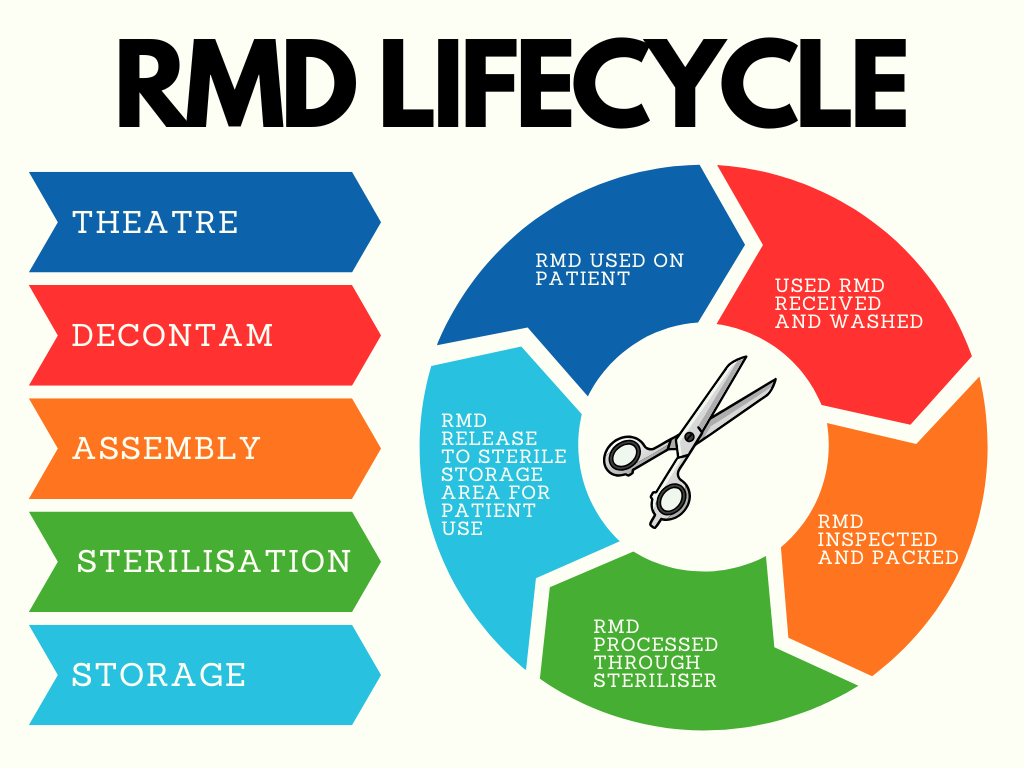
Every surgical procedure depends on the successful reprocessing of reusable instruments. Behind every tray used in theatre is a complex workflow managed by CSSD teams, including:
- Decontamination and cleaning
- Inspection and assembly of instrument sets
- Packaging and sterilisation
- Quality assurance and distribution
In Australia, these processes are governed by AS 5369:2023 Reprocessing of reusable medical devices (RMDs) standard, the national standard for cleaning, disinfecting and sterilising reusable medical devices. The standard sets requirements for safe reprocessing, storage, handling and traceability of surgical instruments used in healthcare.
Compliance with this standard is also linked to accreditation requirements under the National Safety and Quality Health Service Standards, which require healthcare organisations to have safe and consistent processes for reprocessing reusable equipment.
Put simply, safe surgery cannot occur without effective sterile processing.
Why the Divide Happens
The tension between CSSD and theatres rarely comes from individuals. More often, it is the result of structural challenges within hospital systems.
- Visibility of Work
CSSD work largely happens behind the scenes. Theatre staff see the immediate pressure of a surgical list, while sterile services teams manage the detailed processes required to ensure instruments are safe for reuse.
- Communication Gaps
List changes, loan instruments, or incomplete instrument returns can disrupt the entire reprocessing workflow if not communicated early.
- Time Pressure
Operating theatres are among the most time-sensitive areas in healthcare. When surgical schedules shift rapidly, the impact is often felt downstream in CSSD.
The result can become an “us vs them” mindset, even though both teams share the same objective.
The Cost of Poor Collaboration
When communication between CSSD and theatres breaks down, the effects can ripple throughout the hospital.
Potential consequences include:
- Delayed surgical lists
- Increased staff stress and burnout
- Instrument shortages or duplication
- Reduced theatre efficiency
- Increased operational costs
Australian healthcare guidance emphasises the importance of traceability and coordinated processes for reusable instruments to ensure patient safety and infection prevention.
Without collaboration, even well-designed systems can struggle.

Moving from “Us vs Them” to One Surgical Team
Hospitals that actively strengthen collaboration between CSSD and theatre teams often see measurable improvements in workflow and staff satisfaction.
Some practical strategies include:
Cross-department education
Shadow days between CSSD and theatres help teams understand each other’s pressures and workflows.
Clear communication protocols
Structured processes for surgical list changes, loan sets, and urgent requests reduce last-minute pressure.
Technology and traceability
Digital instrument tracking systems improve transparency across departments and support compliance with traceability requirements under Australian safety standards.
Leadership alignment
Strong collaboration between perioperative and CSSD managers is critical to creating a unified surgical service.
A Shared Goal: Safer Surgery
Whether working in theatre or sterile services, every professional involved contributes to the same outcome: safe surgery for patients.
Standards like AS 5369:2023 reinforce this by highlighting the importance of structured processes, quality systems, and trained staff across the entire instrument lifecycle.
When CSSD and theatre teams recognise their shared role in patient care, the narrative shifts from “CSSD vs Theatre” to “CSSD and Theatre.”
And when that happens, everyone benefits – staff, hospitals, and most importantly, patients.

